Post Updated February 7, 2022
For the large majority of us who suffer one or more symptoms of menopause, we can all agree that it is NO FUN.
So what can we do about it?
According to the North American Menopause Society (NAMS), a leading group of health care providers who specialize in health issues for women at perimenopause and beyond, hormone replacement therapy remains the most effective treatment for the symptoms of menopause.
But wait! Isn’t hormone replacement therapy bad for you?
There has been much conflicting information about the benefits and risks of hormone replacement therapy, so we at MiraKind want to try to dispel the myths and sort through the noise so that you can make a clear and informed decision for yourself.
What is hormone replacement therapy (HRT)?
Hormone replacement therapy (HRT) supplements a woman’s estrogen levels during perimenopause and menopause, helping diminish the unpleasant symptoms—night sweats, hot flashes, vaginal dryness, sleep disturbance—that result from decreasing estrogen levels. HRT can be taken in various forms—pill, patch, gel, spray—and either given as estrogen alone (typically used for women who have had a hysterectomy) or combined with progestin for women who still have their uterus (progestin is protective against risk of uterine cancer when estrogen is used alone).
Talk with a menopause-specialist doctor about HRT to learn more about the risks and benefits – you may even be able to get a prescription online by speaking with a genneve menopause specialist via video appointment.
Why has HRT gotten such a bad rap?
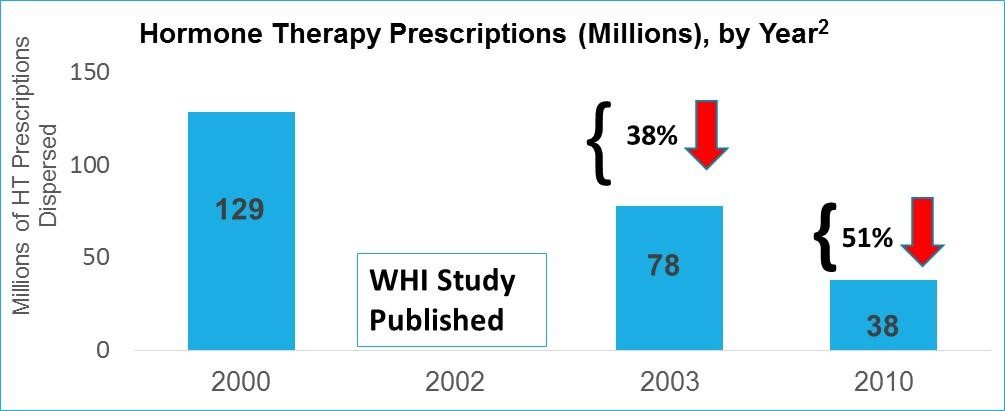
Hormone replacement therapy has gotten a bad rap, in large part due to the Women’s Health Initiative (WHI) study published in 2001. The WHI indicated that hormone replacement therapy led to increased breast cancer risk, increased risk of stroke, and blood clots, among other health issues. When the WHI study findings came out, HRT usage among peri- and menopausal women plummeted, and has yet to recover, even 16 years later. However, the study was found to be plagued with several flaws that were corrected in later studies. Still, confusion remains. According to the NAMS 2012 position statement on HRT use, “Ten years have passed since the publication of the first results of the Women’s Health Initiative (WHI) hormone therapy trials. The debate that followed gave women and their providers the impression that the experts don’t agree on the topic of hormone therapy.” 1
So is HRT OK for me to use or not?
The ultimate conclusion, with consensus by the North American Menopause Society, Society for Reproductive Medicine, and the American the Endocrine Society, is that “most healthy, recently menopausal women can use hormone replacement therapy for relief of their symptoms.” 1 Scientists who conducted a 13-year, long-term follow-up of WHI participants concurred, reporting in 2015 that, “For most recently menopausal women, benefits of HRT outweigh the risks.” In short, hormone replacement therapy is not a one-size-fits all solution, and the decision to take it should take into account numerous factors, including a woman’s health and family history, the severity of her symptoms, age of menopause, etc.
How do I know if HRT is right for me?
A 2015 MiraKind survey of 600 women showed that 60% expressed concern or a lack of clarity around HRT and 50% of women surveyed believe that HRT increases cancer risk. Clearly, there is still a lot of confusion and misunderstanding around the topic, so how do you decide whether it is right for you?
While there are many factors to consider, understanding your genetic profile can prove invaluable in your decision-making process. Joanne Weidhaas, MD, PhD, and her colleagues published research in 2015 that pointed to estrogen withdrawal—which occurs during menopause, abrupt stoppage of HRT, or a pre-menopausal oophorectomy without HRT—as a potential trigger for the onset of cancer in women who carry an inherited genetic mutation known as the KRAS-variant. For women who do test positive for the KRAS-variant, maintaining one’s estrogen levels via hormone replacement therapy through peri-menopause and into menopause appears to be protective in decreasing cancer risk.
While any decision around prescription HRT should involve a consultation and discussion with your physician, if you are a woman experiencing menopausal symptoms and are trying to decide whether to go on or stay on HRT, you may want to consider getting tested for the KRAS-variant. Regardless of whether you test positive or negative, the result will provide you with a powerful piece of genetic information to help inform this important decision about your health.
Recommended Reading: “Women Have Been Misled About Menopause”, by Susan Dominus, New York Times Magazine, February 2023.
Learn more about menopause and the KRAS-Variant.
Learn more about our latest research on estrogen and how it impacts the KRAS-variant.
Resources:
- The Experts Do Agree about Hormone Therapy: The North American Menopause Society
- https://www.menopause.org/docs/for-women/expertsagree_consumer.pdf
- http://www.medscape.com/viewarticle/850634




Leave a Reply