
In last February’s blog, we looked at how menopause relates to heart health and how menopausal hormone therapy (MHT), also known as hormone replacement therapy (HRT), can protect against heart disease risk in some women. Since then, new analyses and regulatory changes have reshaped the current view of hormone therapy.
In 2025, the FDA removed the black box warnings from MHT. This decision followed years of evidence showing that many of the suggested risks of MHT were outweighed by the benefits, including those around cardiovascular health.
This article reviews what is now understood about estrogen and the heart and how the timing of estrogen replacement therapy impacts heart health. It also examines how differences in estrogen exposure—including type, delivery, and dose—meaningfully influence cardiovascular outcomes, with modern non-oral MHT showing favorable cardioprotective effects.
How estrogen protects the heart
Before menopause, estrogen protects the heart and blood vessels in several very important ways:
- Blood vessel flexibility
- Keeps arteries more relaxed and responsive, which supports steady blood flow.1,2
- Cholesterol balance
- Slows plaque buildup in the arteries by increasing HDL (“good” cholesterol) levels and lowering LDL (“bad” cholesterol) levels.3,4
- Vessel inflammation
- Quiets inflammatory activity inside blood vessels that can contribute to damage over time.2,3
- Oxidative stress
- Reduces damage from reactive molecules that affect blood vessels and heart cells.2,5
- Heart tissue structure
- Appears to limit the stiffening and scarring of the heart muscle.4,6
Long before the science behind these protective effects of estrogen for women’s hearts was understood, researchers noticed a consistent pattern: women generally developed heart disease later than men, with risk starting to increase around menopause.7 As estrogen levels dropped and women’s risk rose, it became clear that estrogen had been offering protection during pre- and perimenopause.7
Correlation Between Menopause and Heart Disease
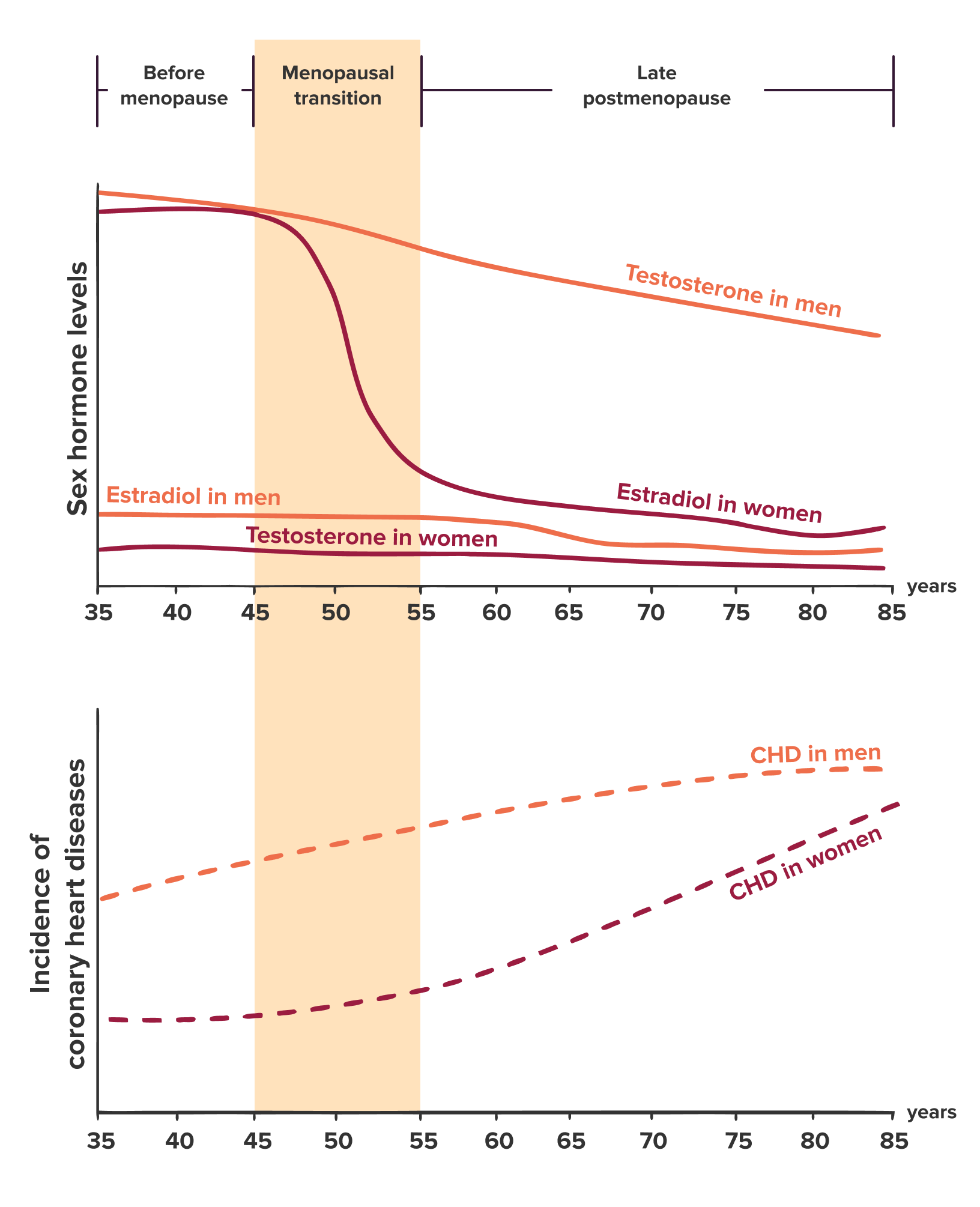
Coronary heart disease (CHD) by age in men and women. Men typically develop heart disease earlier in life. Women’s risk remains lower until around the time of menopause, after which it increases and begins to approach men’s risk levels. Adapted from Davezac et al., Estrogen Receptor and Vascular Aging, Frontiers in Aging, 2021, CC BY 4.0. Original figure adapted from Lerner & Kannel, 1986.
Early observational studies also reported lower rates of heart disease among women taking MHT, suggesting that estrogen, in the form of MHT, may actually help prevent cardiovascular disease for postmenopausal women.
When caution impacted practice
However, these observations and beliefs about the protective role of estrogen and MHT in heart health came into sharp focus in the early 2000s with the Women’s Health Initiative (WHI). Among the many negative findings regarding MHT in the study, they found that MHT led to higher rates of coronary heart disease, heart attacks, and strokes.8,9 The response to this news was swift. Primarily out of fear of “increased” breast cancer risk, many women abruptly stopped hormone therapy, and many clinicians became reluctant to prescribe it.
The sudden drop in MHT use didn’t just change prescriptions; it changed women’s health outcomes. Researchers soon began asking an important question: what happened to women’s heart health after so many stopped estrogen so quickly?
A 2013 study looked at the impact of the sharp decline in estrogen use following the WHI study on heart health. For context, before the WHI study, over 90% of women in their 50s who had undergone hysterectomies were using estrogen therapy.10-12 Because of the widely communicated results of the WHI study, use dropped dramatically. Over the following decade, the researchers modeled the potential impact and estimated that avoiding estrogen among these women may have contributed to tens of thousands of excess premature deaths—possibly as many as 90,000 overall—with cardiovascular disease accounting for most of them.13
So, what, then, is the truth about MHT and heart health? And why did the WHI study find what it did? To answer this, we must compare differences in estrogen timing and exposure in the WHI study to how MHT is offered today.
MHT timing and cardiovascular risk
In the WHI study, women started MHT between the ages of 50 and 79, with an average age of 63. Because most women enter menopause around age 50, many participants were more than ten years past menopause when therapy began. The initial report found higher overall rates of cardiovascular problems, but it did not break the results down by age.
The timing hypothesis
We now know that the impact of estrogen on the heart depends on both a woman’s age and the number of years since menopause. This is known as the timing hypothesis.14 This concept can help explain why estrogen affects the heart differently at various times after menopause.
At the start of menopause, arteries are often still relatively healthy. Plaque buildup is usually minimal, and blood vessels remain flexible. Starting estrogen at this time can support heart health and slow the changes linked to estrogen loss that increase cardiovascular risk.14
But as more years pass, blood vessels become rigid, and plaque accumulates, often without leading to obvious symptoms. Starting estrogen at an older age might cause existing plaques to be less stable and break away, raising the risk of blood clots or other cardiovascular events and actually causing harm.14-17
Applying the timing hypothesis to the WHI data in a 2025 reanalysis study found that the effects of estrogen depended on a woman’s age and the number of years since the start of menopause, as shown below.
Health Effects of Menopausal Hormone Therapy by Age17
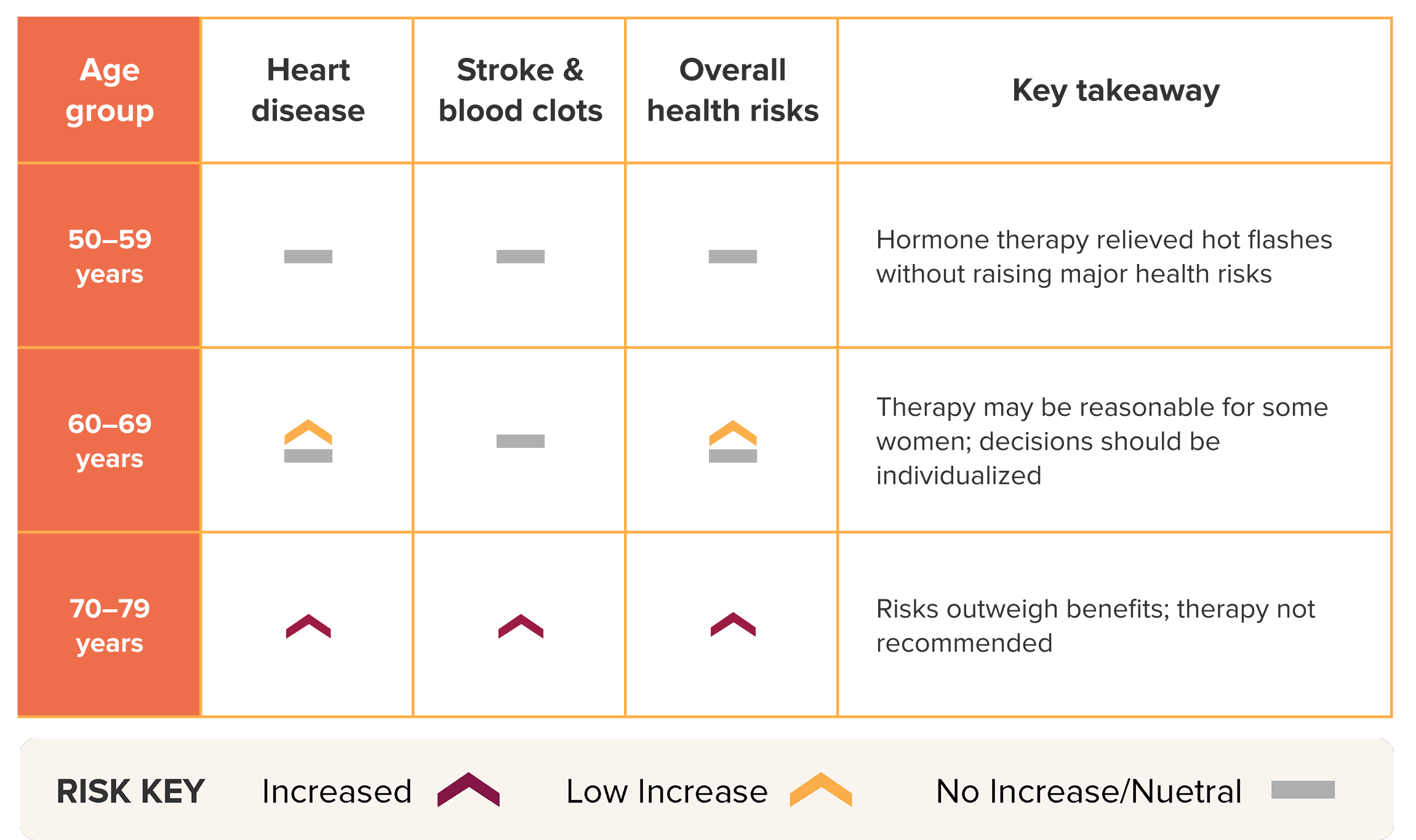
Other trials, including KEEPS18 and ELITE19, show similar patterns, with low cardiovascular risk if estrogen therapy begins before age 60 or within ten years of menopause.
Does such evidence mean that women over 60 should not take MHT to relieve hot flashes and night sweats? Not necessarily, as this will vary by individual, and there is more to the story.
Estrogen exposure and the liver
It turns out that timing isn’t the only factor that can impact heart health—estrogen exposure is just as important. Estrogen exposure refers to the type of estrogen used, how it’s delivered, and the dose.
The WHI study used the most commonly prescribed form of estrogen at the time: a high dose of oral conjugated equine estrogens (CEE), a mixture of roughly 10 different estrogens derived from the urine of pregnant horses.20 Importantly, oral estrogen is first broken down by the liver before entering the bloodstream—a process called first-pass metabolism. As a result, the liver produces higher-than-normal levels of proteins involved in blood clotting and inflammation, which is known to increase the risks of blood clots, stroke, and heart attack.21-23
First-Pass Metabolism
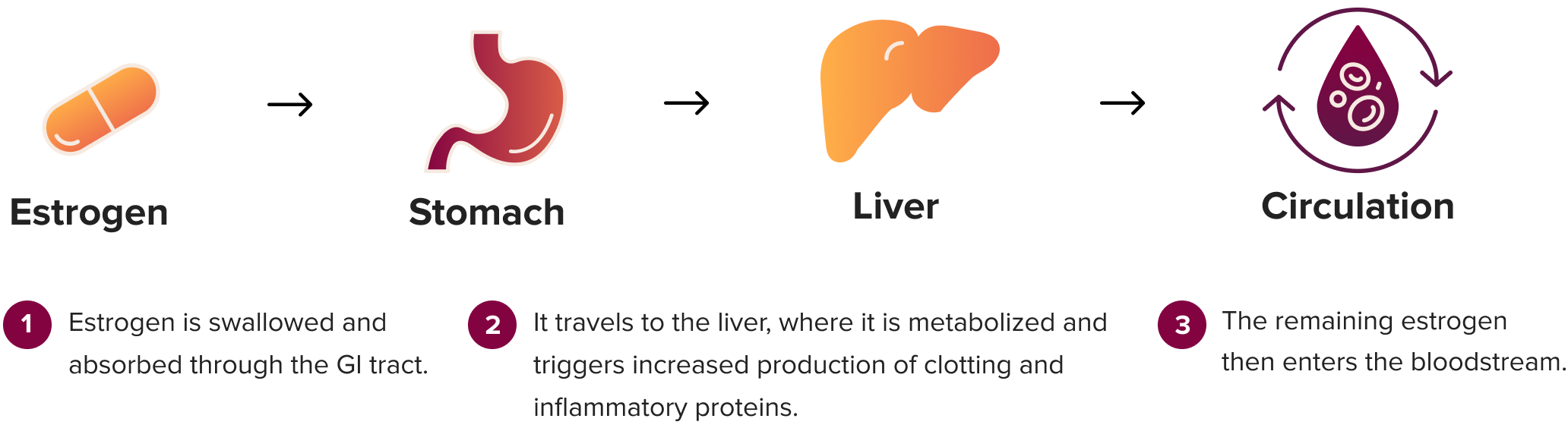
This is all very different from what is prescribed today: 17β-estradiol, a bioidentical estrogen that is identical to what our body produces. It is available in both non-oral and oral forms. Oral 17β-estradiol still undergoes first-pass metabolism but has less “liver effect” than CEE, because CEE contains several different estrogens that require more extensive liver processing.24-26
Non-oral estrogen options—patches, gels, or vaginal products—are commonly prescribed for MHT and bypass first-pass metabolism in the liver. As a result, they have little to no effect on clotting or inflammation and generally pose very low, if any, cardiovascular risk.27-36 In addition, because they enter the bloodstream directly, they are used at lower doses, which are just as effective as higher-dose pills for relieving hot flashes and night sweats.
The table below highlights findings from studies comparing oral and non-oral estrogen use and their implications for cardiovascular health.
Estrogen Exposure and Cardiovascular Health
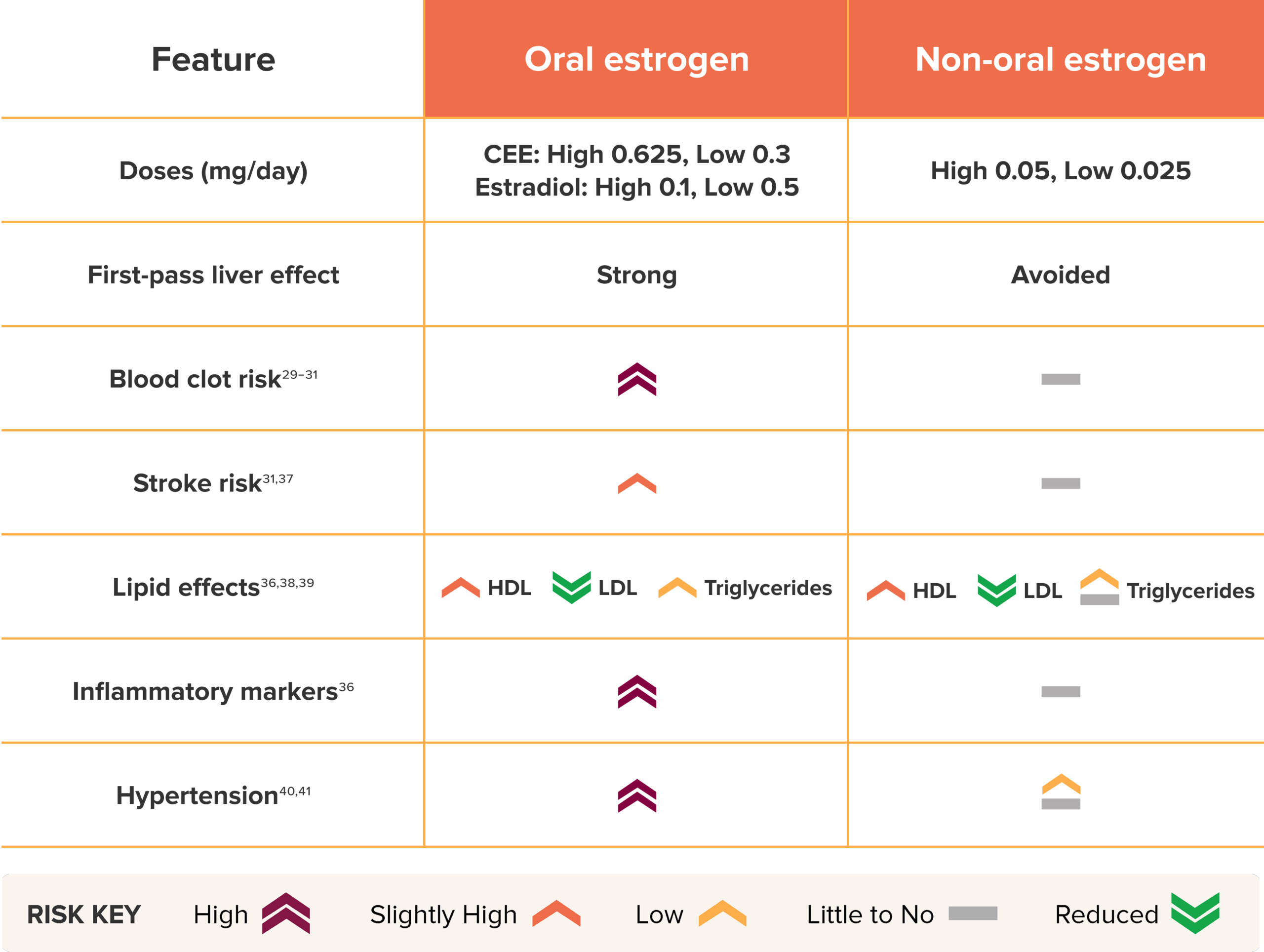
Modern MHT and Cardiovascular Risk
When examined in large real-world populations, differences in estrogen exposure meaningfully influence cardiovascular risk, with non-oral estrogen associated with a favorable cardiovascular risk profile.
A large UK study published in The BMJ examined over 80,000 women aged 40–79 who developed venous thromboembolism (VTE), a serious blood clot, and compared them with over 390,000 women in the same age range who did not. Oral therapies were associated with a 58% increased risk of VTE, while patches and gels did not increase risk, no matter the dose. And when the two different types of oral treatments were compared, estradiol carried a lower risk than CEE: 22% versus 40% for low doses and 35% versus 71% for high doses.42
Additionally, a large 2024 observational study of over 10 million Medicare beneficiaries aged 65 and older found that women using non-oral estrogen compared to oral estrogen had:43
- 5% lower risk of heart failure
- 3% lower risk of blood clots
- 11% lower risk of heart attack
Even for women taking estrogen with progestin, non-oral forms of estrogen were linked to better heart outcomes than oral estrogen.43
In closing
Although the WHI study was designed to test whether MHT prevented heart disease and improved overall long-term health outcomes in postmenopausal women, it did not factor in the timing hypothesis, nor did it look at liver-mediated clotting risks. All of the findings discussed here suggest that, for healthy women, MHT is likely safe and even protective for the heart when the type, dose, and method of delivery are appropriately chosen using current-day products and understandings.
What we now know is more reassuring. For women under 60, or within about ten years of menopause, today’s menopausal hormone therapy, especially the non-oral delivery approaches, supports heart health. The FDA’s 2025 decision to remove black box warnings reflects this clearer understanding.
Hormone therapy is not the right choice for every woman. But avoiding it solely because of older interpretations no longer matches the evidence. In some cases, women well past their 60s or even into their 70s may still be appropriate candidates. Decisions are best guided by current knowledge and individual health, rather than lingering fears from the past.
Read the February 2025 blog: Does MHT Lower Heart Disease Risk? The Truth About Estrogen
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9005843/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3972065/
- https://www.mdpi.com/1422-0067/21/12/4314
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5688223/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8260319/
- https://www.ahajournals.org/doi/10.1161/circresaha.110.236687
- https://pubmed.ncbi.nlm.nih.gov/970770/
- https://jamanetwork.com/journals/jama/fullarticle/195120
- https://jamanetwork.com/journals/jama/fullarticle/198540
- https://journals.lww.com/menopausejournal/abstract/2011/04000/trends_in_menopausal_hormone_therapy_use_of_us.9.aspx
- https://onlinelibrary.wiley.com/doi/10.1002/pds.985
- https://jamanetwork.com/journals/jama/fullarticle/197940
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3780684/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4834454/
- https://www.jacc.org/doi/10.1016/j.jacc.2005.10.076
- https://www.fertstert.org/article/S0015-0282%2804%2903019-5/fulltext
- https://pubmed.ncbi.nlm.nih.gov/40952729/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6738629/
- https://www.nejm.org/doi/full/10.1056/NEJMoa1505241
- https://pubmed.ncbi.nlm.nih.gov/24176763/
- https://www.frontiersin.org/journals/endocrinology/articles/10.3389/fendo.2025.1617731/full
- https://pubmed.ncbi.nlm.nih.gov/18303079/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC2684668/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4636198/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5371691/
- https://www.sciencedirect.com/science/article/pii/S0735109703001566
- https://www.sciencedirect.com/science/article/abs/pii/S0049384811700081
- https://pubmed.ncbi.nlm.nih.gov/26544651/
- https://pubmed.ncbi.nlm.nih.gov/20601871/
- https://pubmed.ncbi.nlm.nih.gov/30358726/
- https://pubmed.ncbi.nlm.nih.gov/20670199/
- https://pubmed.ncbi.nlm.nih.gov/33506261/
- https://journals.lww.com/menopausejournal/abstract/2016/06000/venous_thromboembolism_and_cardiovascular_disease.5.aspx
- https://pubmed.ncbi.nlm.nih.gov/26953655/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12511246/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8063246/
- https://journals.lww.com/menopausejournal/abstract/2026/02000/efficacy_of_oral_versus_transdermal_estrogen.16.aspx
- https://www.ahajournals.org/doi/10.1161/strokeaha.117.017132
- https://www.nejm.org/doi/10.1056/NEJM199110243251702
- https://newsroom.heart.org/news/women-taking-oral-estrogen-hormones-may-have-increased-risk-of-high-blood-pressure
- https://pubmed.ncbi.nlm.nih.gov/25268408/
- https://www.bmj.com/content/364/bmj.k4810
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11465799/




Leave a Reply