This post explores BRCA variants vs. the KRAS-variant and is part two of our series on understanding the different genetic causes of cancer.
In part one of our series, we compared genetic variants and mutations, specifically the KRAS-variant and KRAS mutations.
Quick recap on genetics and cancer development
In our last blog post, we learned that cancer results from genetic differences you are born with (variants) or genetic changes to your DNA that happen over your lifetime (mutations).
Understanding genetic variants
Genetic variants that can lead to diseases, like cancer, are called pathogenic variants. While they may often be called mutations (i.e., BRCA mutations), they are technically pathogenic variants.
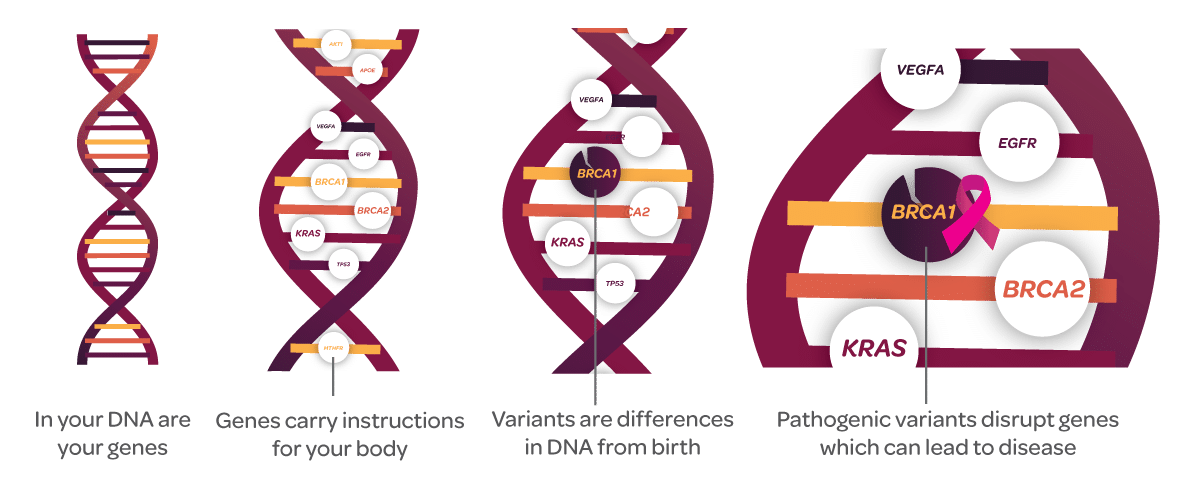
Our DNA is full of genetic variants, or differences you are born with. However, where the variant is located in your DNA can have a big impact on the variant being a meaningless difference, or one that can increase your risk of disease. For example, variants in or near genes are more likely to be pathogenic. Genes are small parts of your DNA that contain instructions for your body and each gene has a control center. BRCA and KRAS are examples of genes everyone is born with.
Both BRCA and KRAS are genes that can be disrupted by pathogenic variants. There are two known BRCA genes with pathogenic variants linked to cancer: BRCA1 and BRCA2. The KRAS-variant is also a pathogenic variant associated with cancer, and it affects the control center of the KRAS gene.
Key Terms
- BRCA1, BRCA2 & KRAS – genes everyone is born with
- Gene – a small part of DNA from your parents
- Variant – an inherited difference in a gene or a gene’s control center
- Pathogenic Variant – an inherited difference in a gene or a gene’s control center that is linked to disease
BRCA variants vs. the KRAS-variant
While BRCA variants and the KRAS-variant are all pathogenic variants, they are different.
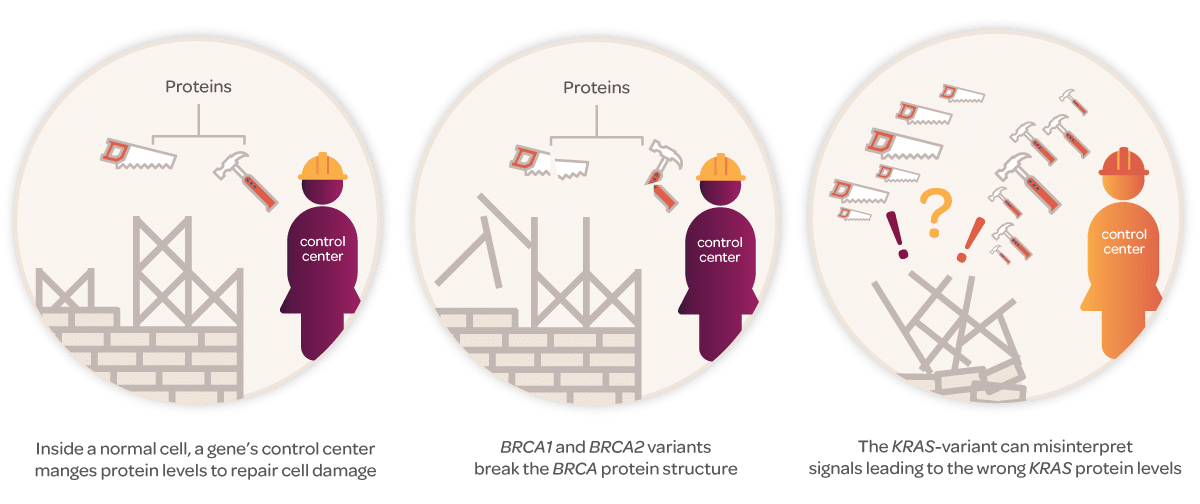
The main difference between pathogenic BRCA variants and the KRAS-variant is where they are in the DNA, which impacts how they work. BRCA variants affect the protein the BRCA gene makes, which performs vital functions within our cells. However, the KRAS-variant affects the KRAS control center, which manages the levels of KRAS protein the gene makes.
While a BRCA variant patient may be unable to make normal BRCA protein to repair damage in cells, the KRAS control center in a KRAS-variant patient may misinterpret signals and make the wrong amounts of the KRAS protein, leading to mismanaged cell growth — both of which can lead to the development of cancer.
BRCA variants are more well-known than the KRAS-variant
Thanks to Angelina Jolie, many people have heard of the BRCA variants and their connection to breast and ovarian cancer. In contrast, the KRAS-variant is relatively unknown, even though it is associated with breast, ovarian and lung cancer.
The KRAS-variant is more prevalent than BRCA variants
The KRAS-variant is found in up to 25% of breast and ovarian cancer patients, making it far more common than pathogenic BRCA variants, which are found in only up to 5%.
BRCA variants and the KRAS-variant are associated with increased cancer risk, specifically breast and ovarian
The breast cancer risk for women with:
- BRCA1 is 55%–72%*
- BRCA2 is 45%–69%*
- The KRAS-variant is 25%-30%
The ovarian cancer risk for women with:
- BRCA1 is 39%–44%*
- BRCA2 is 11%–17%*
- The KRAS-variant is 10%-12%%
*Stats on BRCA from cancer.gov
While people are born with these pathogenic variants, there are things they can do to reduce their risk of cancer.
As the BRCA variants affect the way the BRCA protein is made in a cell, there is not much that can be done to influence or change them. Patients can enhance their breast and ovarian screening and/or get surgery to remove the areas at risk of developing cancer. Surgeries may include a double mastectomy, an oophorectomy (ovary removal surgery), or a hysterectomy.
Since the KRAS-variantis a genetic variant in the control center of KRAS, it responds to other signals, like a woman’s estrogen decline in menopause. Our research has shown that healthcare choices to change any triggering factors can decrease a KRAS-variantpositive person’s risk of cancer. Therefore, individuals with the KRAS-variantcan use strategies other than surgery to prevent cancer, like menopausal hormone therapy.
Finding out if you’re at an increased risk for cancer based on your genetics is potentially life-saving.
If you’d like to either find out if you have the KRAS-variant or help further our research of this unique type of genetic variant, you can learn more here.



Leave a Reply