
Most people think of BRCA genes as a women’s health issue, linked to breast and ovarian cancer. But they affect men too, as men are just as likely to have BRCA mutations. And it turns out that alterations in these genes do matter for men, as they can increase the chance of developing aggressive prostate cancer.
In this post, we’ll talk about what BRCA genes do, what happens when they are mutated, and how sometimes this can increase the risk of aggressive prostate cancer. We’ll also look at new treatments, including PARP inhibitors, that specifically target tumors with BRCA mutations.
What are BRCA genes?
BRCA stands for “BReast CAncer susceptibility gene” and refers to two genes found in everyone: BRCA1 and BRCA2. Although named because of their discovered association with breast cancer risk, these genes themselves do not cause breast cancer.1,2 In fact, they protect cells from becoming cancerous. They do this by encoding proteins that repair a type of DNA damage called double-stranded breaks.3 This damage can happen naturally in rapidly growing and dividing cells, or when molecules called free radicals damage DNA, among other causes.4
BRCA protein helps repair damaged DNA
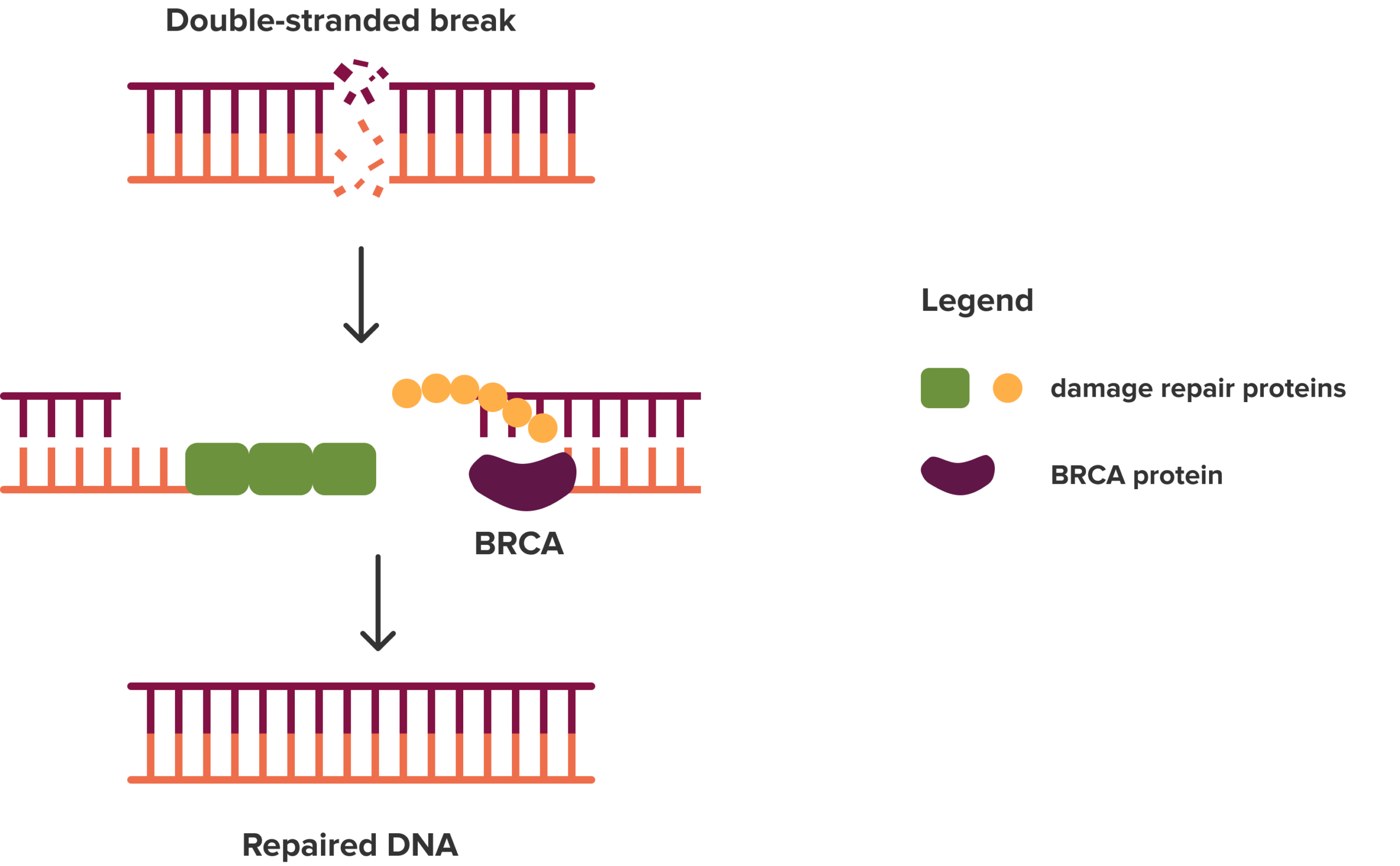
Sometimes DNA suffers serious breaks in both strands, called double-strand breaks. The BRCA1 and BRCA2 proteins, along with other proteins, help repair these dangerous breaks. Figure adapted from Mangogna A. et al., “Homologous Recombination Deficiency in Ovarian Cancer: from the Biological Rationale to Current Diagnostic Approaches,” Journal of Personalized Medicine 2023;13(2):284, https://doi.org/10.3390/jpm13020284, CC BY 4.0.
BRCA and Cancer Risk
People who have a BRCA1 or BRCA2 mutation, or in other words, a BRCA gene that is not working normally, can have an increased risk of developing breast, ovarian, prostate, or pancreatic cancer compared to the general population.
Approximate cancer risks by BRCA1/2 mutation status
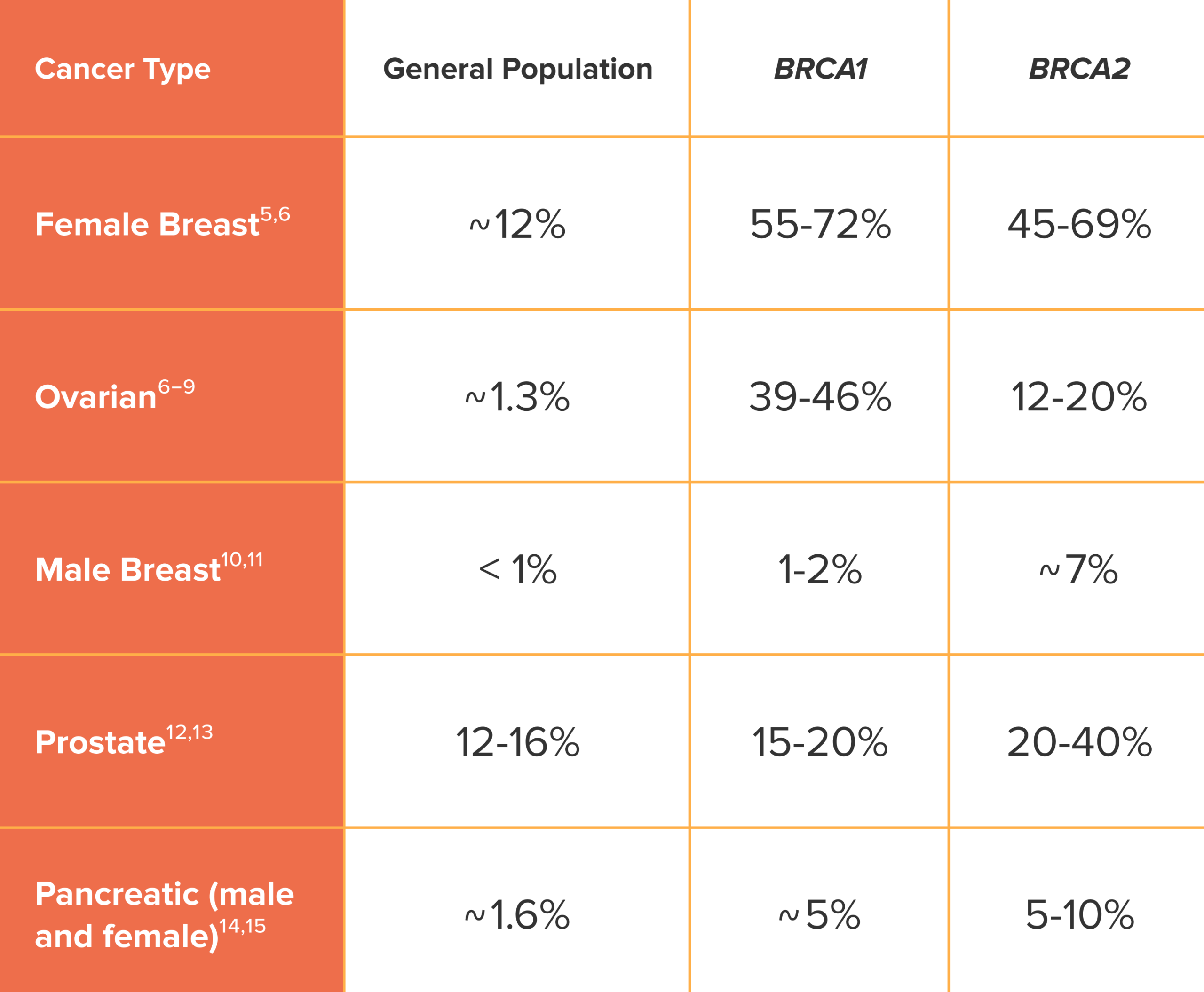

Although BRCA mutations greatly increase breast cancer risk in women, they rarely do so in men. It is also notable that BRCA1 mutations barely increase prostate cancer risk in men, while BRCA2 mutations roughly double it. However, BRCA mutations are still very important in prostate cancer, as discussed later in this post. But first, why do BRCA mutations affect certain tissues, such as the breast, ovaries, and prostate, more than others?
Breast, ovary, and prostate and why they are affected by BRCA mutations
To try to answer this question, let’s revisit what BRCA genes do. They encode proteins that repair damaged DNA. When they aren’t working properly, damage can build up, which raises the chance of cancer. This is especially true in organs with rapid cell turnover, particularly hormone-sensitive tissues.16-18
Women experience a lifetime of hormonal fluctuations, especially estrogen, that affect their breasts and ovaries, from monthly cycles to pregnancy and menopause. These periods of rapid cell division make breast cells and ovarian surface cells more likely to accumulate damage if a BRCA protein isn’t functioning properly, increasing the risk of cancer.16,19,20
Men, by contrast, have much higher testosterone and produce little estrogen, so their breast tissue stays relatively unchanged throughout life. The prostate, however, undergoes rapid cell division driven by testosterone. When a defective BRCA protein impairs DNA repair, the damage can build up in the prostate and increase the risk of cancer.23
BRCA and prostate cancer
Although BRCA2 mutations do increase the risk of prostate cancer, most men diagnosed with the disease do not have it. Studies show that only about 1–2% of men with localized prostate cancers are found to have a BRCA mutation.21,22
Because these mutations are relatively uncommon and their impact on developing prostate cancer is low, it is not standard to test people for BRCA mutations to determine if they are at higher risk of prostate cancer. However, BRCA genetic testing may be considered for men with the following risk factors:
- A BRCA mutation in the family, especially BRCA2
- Two first- or second-degree relatives with breast, pancreatic, or prostate cancer, suggesting there might be a BRCA2 mutation in the family
- Having a father or brother diagnosed with prostate cancer
- People of Ashkenazi Jewish descent
For men who are found to carry a BRCA mutation, prostate cancer screening begins at around age 40, ten years earlier than for the general population.
Early detection for this group of men can be important since men with a BRCA2 mutation are more likely to develop aggressive metastatic prostate cancer, as explained below.
Progression of advanced prostate cancer
Prostate cancer generally goes through set stages. The first stage is localized disease, typically treated with surgery or radiation therapy. If the cancer progresses despite these treatments, it can become metastatic, meaning it has spread outside of the prostate. When it first spreads, it usually begins as metastatic castration-sensitive prostate cancer (mCSPC). At this stage, anti-testosterone therapies are still effective in controlling the disease.
However, if the cancer progresses, it can become resistant to anti-testosterone treatments and is then referred to as metastatic castration-resistant prostate cancer (mCRPC). mCRPC is the most advanced form of prostate cancer and is more difficult to treat, with a median survival of only about three years.23,24 Men with BRCA2 mutations are more likely to progress to this stage, and roughly 5–6% of men with mCRPC have the mutation.13,25
Because of this, researchers have been looking for new ways to target BRCA-mutated prostate cancers more effectively.
Progression of prostate cancer that does not respond to therapy

Advanced therapy for prostate cancer in BRCA mutant patients: PARP inhibitors
Our cells rely on multiple systems to repair DNA damage. BRCA proteins repair one of the most serious types, double-stranded breaks, while poly ADP-ribose polymerase (PARP) proteins repair single-strand breaks. These different repair pathways work together to keep DNA intact and maintain healthy cells. A new class of drugs prevents PARP from working, and they are called “PARP inhibitors.”
PARP inhibitors and how they work in tumors with BRCA mutations
Every person has two inherited copies of the BRCA1 and BRCA2 genes, one from each parent. If someone inherits a BRCA mutation from a parent, only one copy is affected, while the other can still repair DNA and keep the cell functioning. In a cancer of a patient with a BRCA mutation, the second normal copy of BRCA has often also become damaged through a mutation that occurs after birth, called an “acquired” or “somatic” mutation. This means that the tumor cells have no functional BRCA genes, which is called “BRCA-deficient.”
In addition, inheritance is not the only way that a tumor can become BRCA-deficient. Sometimes, the mutations are not inherited but instead acquired in both copies in a person’s lifetime, which happens more often in prostate cancer than in other cancers. When a tumor is BRCA-deficient, it can’t repair double-stranded breaks. This makes the cancer cells especially vulnerable to PARP inhibitors, which block the alternative DNA repair pathway that fixes single-stranded breaks. As a result, BRCA-deficient tumors respond very well to PARP inhibitors.
How PARP inhibitors work in BRCA-deficient cancer cells
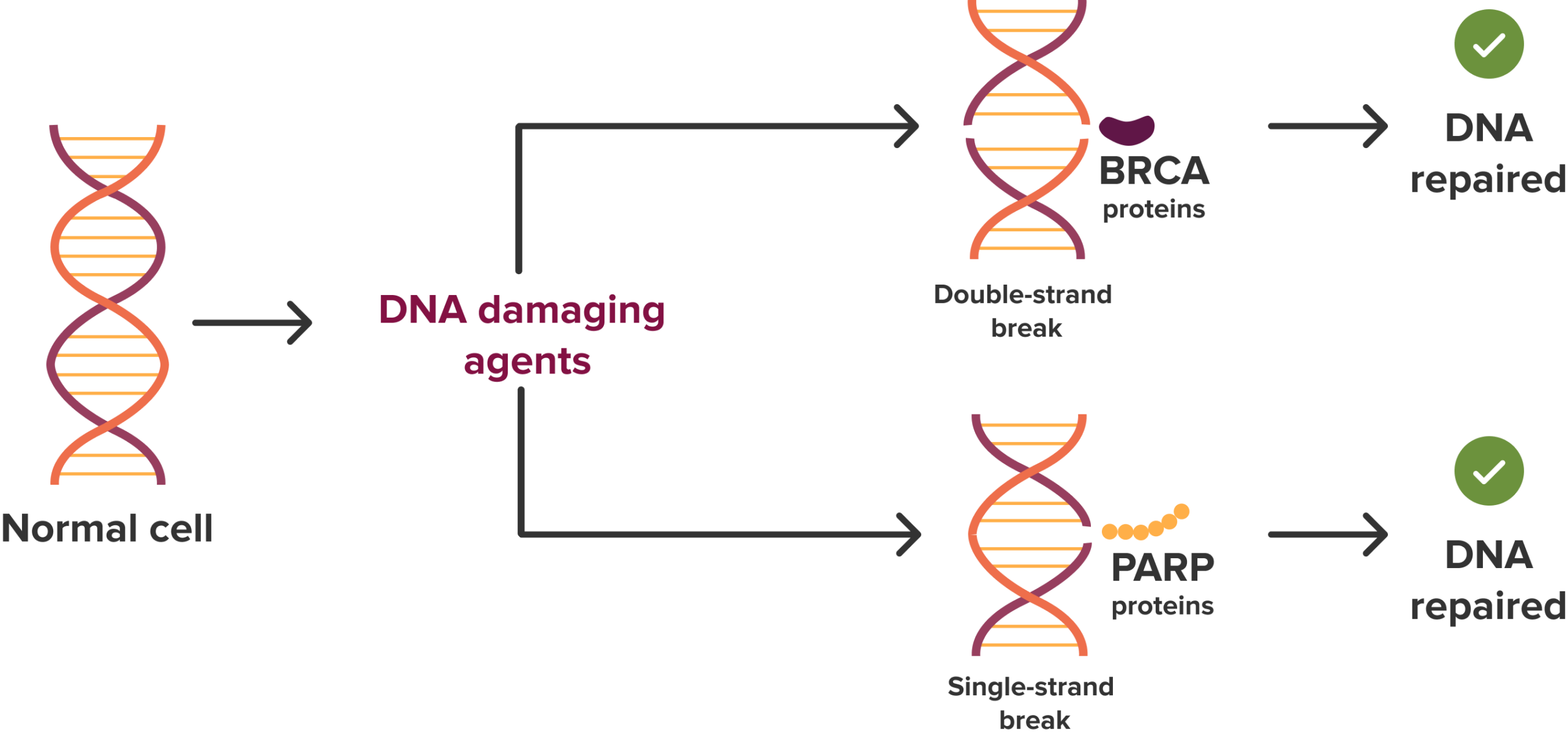
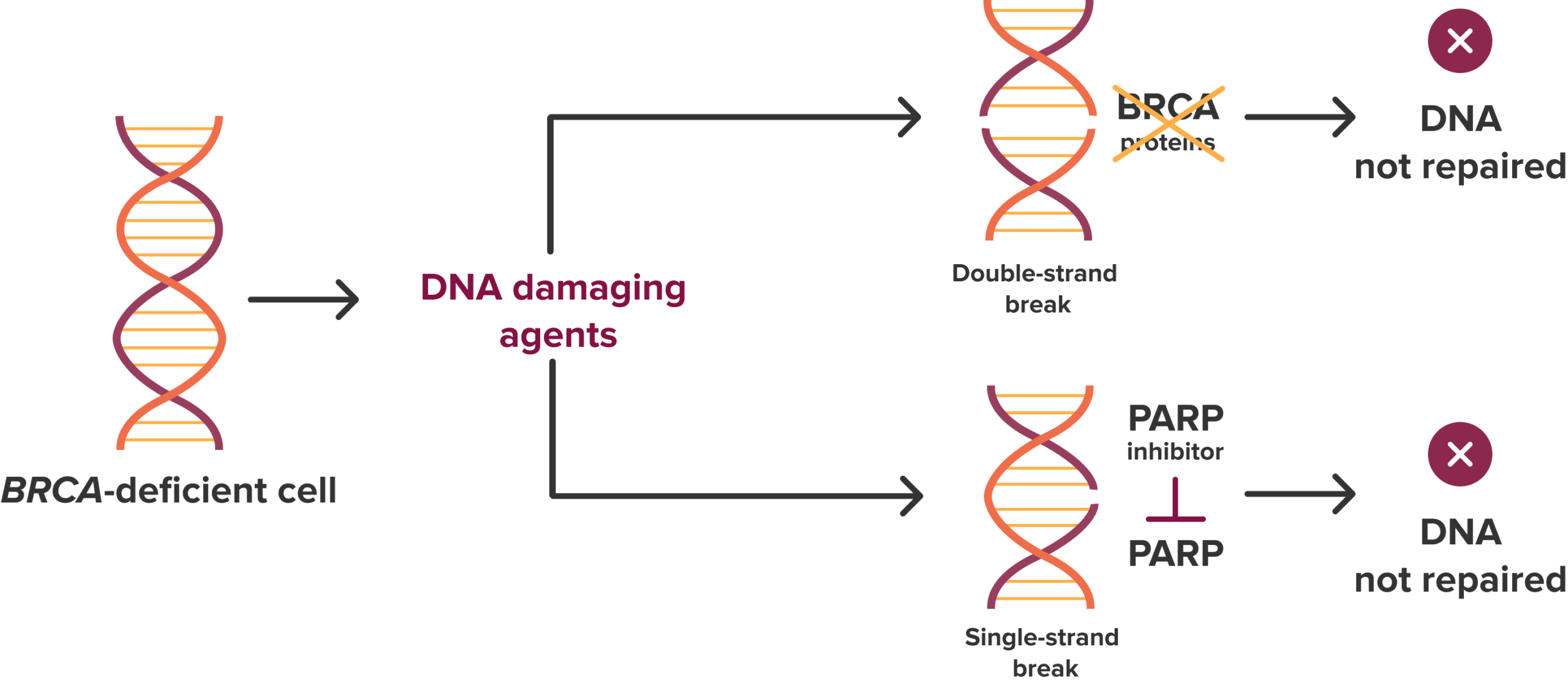
Cells use PARP proteins to repair single-strand breaks in DNA and BRCA proteins to repair double-strand breaks. In patients with BRCA-deficient tumors that are treated with a PARP inhibitor, both single-strand and double-strand DNA repair are impaired, leading to the accumulation of DNA damage and eventual cell death. DNA-damaging agents occur naturally, like free radicals, or by rapid cell division, as mentioned earlier. Figure adapted from Ocana A. et al., “Targeting oncogenic vulnerabilities in triple negative breast cancer: biological bases and ongoing clinical studies,” Oncotarget 2017;8:22218-22234, https://doi.org/10.18632/oncotarget.14731, CC BY 4.0.
Clinical trials and FDA approval of PARP inhibitors
Several clinical trials have tested PARP inhibitors, either alone or in combination with standard treatments, in men with mCRPC who have BRCA1 or BRCA2 mutations. The outcomes across these trials resulted in FDA approval of the drugs in this group of patients with the most advanced form of prostate cancer.
Landmark clinical trials of PARP inhibitors in mCRPC

The success of PARP inhibitors for mCRPC patients sparked research into trying them at an earlier stage of BRCA-deficient prostate cancers.
Targeting BRCA-deficient prostate cancer earlier: PARP inhibitors in mCSPC
It was hypothesized that PARP inhibitors might be effective for BRCA-deficient prostate cancer patients in combination with anti-testosterone treatment when they still had mCSPC, instead of the later stage, mCRPC. Several clinical trials have recently completed testing this hypothesis, and the results look promising.31-33
In one phase 3 study—the AMPLITUDE trial—patients with mCSPC were given the PARP inhibitor niraparib with anti-testosterone hormone therapy abiraterone. The trial found that patients whose tumors had a BRCA2 mutation had a 54% lower disease progression compared to standard care.34 These positive results led to the first FDA-approved PARP inhibitor for the early treatment of BRCA2-deficient mCSPC in December 2025.
Conclusion
BRCA mutations aren’t solely a concern for women; they can also contribute to cancer in men. Understanding how these mutations disrupt DNA repair helps explain why certain tissues, like the prostate in men, are more susceptible. Understanding how BRCA mutations interfere with DNA repair also helps explain why medicine targeting other repair pathways, like PARP inhibitors, can be especially useful. For patients with BRCA mutations and either mCSPC or mCRPC, PARP inhibitors are providing new, personalized treatment options and a chance to extend survival, making this an important step forward in prostate cancer care.
References
- https://www.science.org/doi/10.1126/science.7545954
- https://www.nature.com/articles/378789a0
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4382744/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4142968/
- https://www.cancer.org/cancer/types/breast-cancer/about/how-common-is-breast-cancer.html
- https://jamanetwork.com/journals/jama/fullarticle/2632503
- https://seer.cancer.gov/statfacts/html/ovary.html
- https://jamanetwork.com/journals/jama/fullarticle/2214084
- https://pubmed.ncbi.nlm.nih.gov/29793803/
- https://www.cancer.org/cancer/types/breast-cancer-in-men/key-statistics.html
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5809938/
- https://www.cancer.org/cancer/types/prostate-cancer/detection-diagnosis-staging/survival-rates.html
- https://www.nejm.org/doi/10.1056/NEJMoa1603144
- https://www.mdanderson.org/cancer-types/pancreatic-cancer.html
- https://www.nccn.org/professionals/physician_gls/pdf/genetics_bopp.pdf
- https://academic.oup.com/hmg/article/28/R2/R180/5552778
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4442488/
- https://pubmed.ncbi.nlm.nih.gov/35561581/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6216038/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5216725/
- https://pubmed.ncbi.nlm.nih.gov/30542053/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7492871/
- https://www.mayoclinic.org/diseases-conditions/metastatic-castration-resistant-prostate-cancer/survival-rates/gnc-20593193
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12080741/
- https://pubmed.ncbi.nlm.nih.gov/37173901/
- https://www.nejm.org/doi/full/10.1056/NEJMoa1911440
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7655021/
- https://evidence.nejm.org/doi/full/10.1056/EVIDoa2200043
- https://www.thelancet.com/journals/lancet/article/PIIS0140-6736%2825%2900684-1/abstract
- https://pubmed.ncbi.nlm.nih.gov/40328571/
- https://pubmed.ncbi.nlm.nih.gov/37882449/
- https://ascopubs.org/doi/10.1200/JCO.2025.43.5_suppl.TPS292
- https://ascopubs.org/doi/10.1200/JCO.2025.43.16_suppl.TPS5130
- https://www.urotoday.com/conference-highlights/eau-2026/eau-2026-prostate-cancer/167461-eau-2026-parpi-in-mhspc-or-should-we-wait-until-mcrpc.html



Leave a Reply